Overcoming Peripheral Vascular Disease
Leg pain while walking or resting can feel alarming. It does not have to be a permanent part of your life. Peripheral vascular disease (PVD) reduces blood flow to your limbs, causing discomfort and fatigue. You can manage this condition, stop its progression, and get back to your daily routine without fear.
People often ask about the PVD meaning. It simply refers to diseases of the blood vessels located outside your heart and brain. You might also wonder about the difference between PAD and PVD.One particular kind of PVD that solely affects the arteries is called peripheral arterial disease (PAD). PVD is the broader term that covers conditions affecting both your arteries and your veins.
Reduced blood flow puts your limbs at risk for severe complications. Finding the problem early changes your outcome completely. With the right care plan, you have multiple options for lasting relief and improved mobility.
What Is Peripheral Vascular Disease?
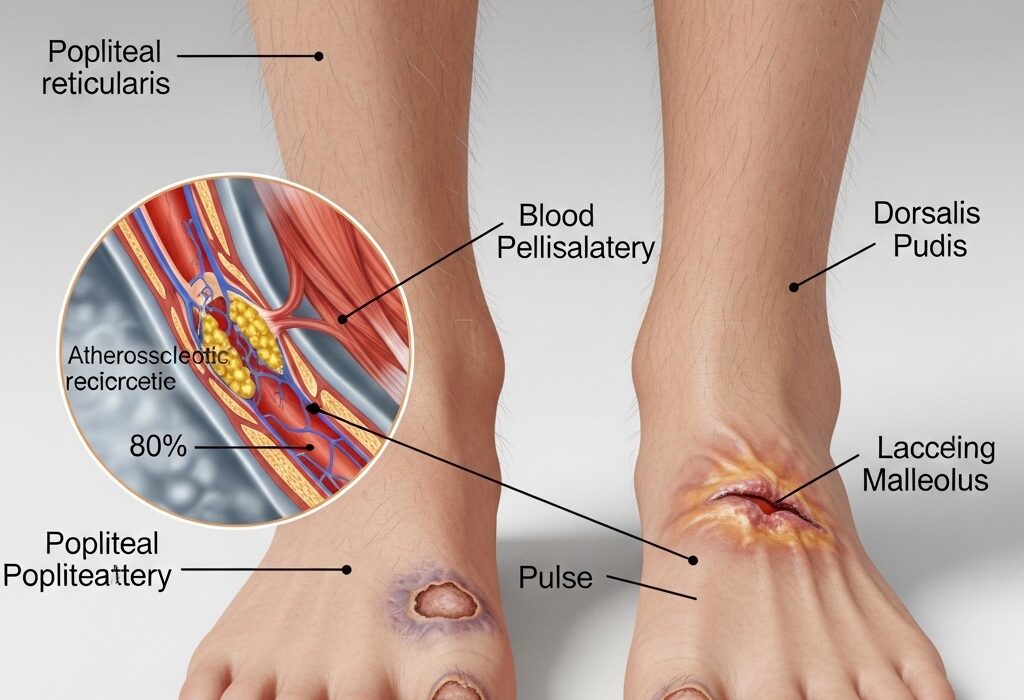
PVD affects the blood vessels outside your heart and brain. It most commonly strikes your legs and arms. Plaque builds up inside your vessels over time. This buildup narrows the pathways.
When your vessels narrow, blood struggles to circulate. Your muscles get less oxygen than they need to function properly. This lack of oxygen causes pain, cramping, and heavy fatigue. The condition affects both the arteries that carry fresh blood away from the heart and the veins that bring used blood back.
Types of Peripheral Vascular Disease
Peripheral Artery Disease (PAD)
PAD blocks the arteries that supply blood to your limbs. Atherosclerosis, or the buildup of fatty plaque, is usually the main culprit.
Peripheral Venous Disease
This condition affects your veins rather than your arteries. Damaged valves cause blood to pool in your legs instead of returning smoothly to your heart.
Functional vs Organic PVD
Organic PVD means physical tissue damage has changed your vessels. Plaque buildup is an organic cause. Functional PVD means your vessels spasm or narrow without physical damage. Cold temperatures, emotional stress, or operating vibrating machinery can trigger these temporary spasms.
Causes of Peripheral Vascular Disease
Understanding peripheral vascular disease causes helps you take control of your health. Atherosclerosis remains the most common cause. Fatty deposits clog your arteries and restrict vital blood flow.
Other common triggers include:
- Smoking
- Diabetes
- High blood pressure
- High cholesterol
- Obesity and a sedentary lifestyle
Symptoms of PVD
Do not ignore leg pain. Vascular disease symptoms often start small but grow worse over time. Catching the signs early prevents severe damage. Common symptoms of peripheral vascular disease in legs include:
- Pain or cramping while walking (claudication)
- Numbness or weakness in the legs
- Coldness in your lower leg or foot
- Wounds or ulcers on your feet that heal very slowly
- Noticeable changes in skin color
- Hair loss on your legs or feet
Risk Factors
Certain factors increase your chances of developing PVD. Age is a primary factor. Your risk goes up significantly after you turn 50.
Smoking damages your blood vessels directly and speeds up plaque buildup. Diabetes impairs blood flow and harms your nerves, making it harder to feel pain in your feet. A family history of heart disease or stroke also raises your risk.
Complications of PVD
Ignoring PVD leads to severe medical problems. One significant risk is critical limb ischemia. This condition causes open sores on your legs or feet that simply do not heal.
Infections can spread deep into the bone and tissue. Severe tissue damage or gangrene may eventually require amputation. Reduced blood flow throughout your body also increases your overall risk of having a heart attack or a stroke.
Diagnosis of Peripheral Vascular Disease
A fast, accurate PVD diagnosis brings peace of mind. Your doctor begins with a simple physical exam to check the pulses in your legs and feet.
They may use an Ankle-Brachial Index (ABI) test. This painless test compares the blood pressure in your ankle to the blood pressure in your arm. A Doppler ultrasound uses sound waves to show blood flow through your vessels. Angiography uses X-rays and a special dye to pinpoint exact blockages. Simple blood tests also check your cholesterol and blood sugar levels.
Treatment Options
Effective PVD treatment focuses on relieving your symptoms and stopping the disease from progressing. You have many highly effective options. When it comes to managing your vascular health, vascular care is the best service provider to guide your recovery safely.
Lifestyle Changes
Small daily habits make a massive difference. Quit smoking immediately. Start a daily walking program to build better circulation in your legs. Eat a healthy diet low in saturated fats and high in fresh vegetables.
Medications
Your doctor may prescribe blood thinners to prevent dangerous clots. Cholesterol-lowering drugs keep plaque from building up further. Blood pressure control medicines reduce the daily strain on your blood vessels.
Medical Procedures
Severe blockages require direct intervention. The best treatment for peripheral vascular disease depends on your specific blockage. Angioplasty and stenting open blocked arteries using a tiny balloon and a wire mesh tube. Bypass surgery creates a new path for blood to flow around the blockage. Thrombolytic therapy involves injecting medicine directly into an artery to dissolve a dangerous blood clot.
Prevention Tips
You can protect your blood vessels. Learning how to prevent peripheral vascular disease starts with your daily choices. Maintain a healthy weight to reduce unnecessary pressure on your circulatory system.
Exercise regularly to keep your blood moving freely. Control your diabetes and blood pressure closely with your doctor. Avoid smoking completely.
When to See a Doctor
Do not wait until the pain stops you from walking. See a doctor right away if you experience persistent leg pain or cramping. Seek immediate help for wounds on your feet that will not heal. Signs of infection, unusual coldness, or skin discoloration require urgent medical attention.
FAQs
What is the difference between PVD and PAD?
PAD affects only your arteries, while PVD affects both your arteries and your veins. PVD serves as the umbrella term for all blood vessel diseases outside the heart and brain.
Is peripheral vascular disease serious?
Yes. Left untreated, PVD increases your risk of severe infections, heart attack, stroke, and potential limb loss.
Can PVD be cured?
Not completely. However, proper medical treatment and targeted lifestyle changes effectively manage symptoms and stop the disease from worsening.
What is the best treatment for PVD?
The most effective approach combines lifestyle adjustments, specific medications, and targeted minimally invasive procedures. Your vascular specialist will design a care plan tailored exactly to your symptoms.
How do you prevent PVD?
Stop smoking and stay active. A healthy diet, regular exercise, and tight control over your blood pressure and blood sugar keep your vessels strong.
Take Control of Your Vascular Health
Peripheral vascular disease limits your movement and threatens your independence. You do not have to accept the pain. Understanding the symptoms and causes is the first powerful step toward healing.
Early diagnosis gives you the best chance at a full, active life. Modern treatments are safe, effective, and prioritize your comfort. Say goodbye to discomfort and take your life back.
Book your consultation today.